Our Hong Kong Foundation Calls for Renewed Efforts to Enhance Access to Mental Health Support
(9 Dec 2022, Hong Kong) Our Hong Kong Foundation (OHKF) called for enhanced access to mental health support in the face of deteriorating mental health of Hong Kong people as shown by the rapidly rising rates of common mental disorders such as depression and anxiety disorder. The OHKF recommends a shift from specialist-focused care model to a community-centric “stepped care” (Figure 1) approach that aligns different levels of support with different healthcare needs.
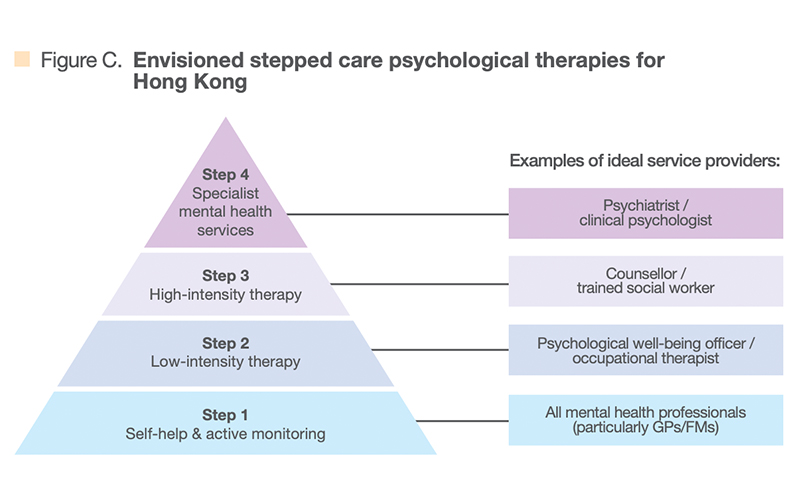
Specialist-level care, encompassing psychiatrists and clinical psychologists, has long served as the default provider of mental healthcare in Hong Kong. This mindset plus manpower shortage have led to a severe bottleneck in mental healthcare delivery, resulting in long delays in accessing professional care and support.
For most CMD (Common mental disorder) patients with mild symptoms, the mental health system needs to build up a wider variety of services, beyond the hospital and specialist setting, and also needs to enhance community level intervention, the Report recommends.
Aligning with the Government’s health policy direction and mental health strategy, the Report explores the potential of implementing stepped mental health care and to improve service accessibility.
The OHKF interviewed over 70 key stakeholders in the mental health field, ranging from policymakers, academics, NGOs, and key health and social care organisations, and also conducted two targeted surveys among community service providers, namely all 24 Integrated Centres for Community Mental Wellness (ICCMWs) and 15 District Health Centres (DHCs) / DHC Expresses (DHCEs). In addition to enhancing community intervention, the Report also recommends enhancing support beyond the formal care system, and enhancing cross-sectoral coordination, collaboration, and governance.
Outside of the hospital and specialist setting, the OHKF advocates leveraging existing resources, such as ICCMWs, DHCs, upskilled counsellors, social workers, and primary care physicians, to offer non-specialist level care. In particular, about 80% of the surveyed ICCMWs agreed that their service model should be reassessed for their role in providing community-based mental health support. Similarly, 60% of surveyed DHC/DHCEs agreed that mental health service provision should be included within their scope of service, with enhanced communication channels to be considered simultaneously between ICCMWs and DHCs.
The Report also calls on the Government to strengthen communication and coordination of multi-disciplinary providers across sectors, such as through assessing the potential use of a more integrated communication platform, enhancing coordination among care providers in the health ecosystem, and developing a common referral assessment and protocol.
To raise public awareness of mental health and encourage help-seeking behaviour, the Report calls for improvement in informal care, namely digital mental health care and workplace intervention.
Digital mental health care covers the continuum of care, from prevention, assessment, intervention to management of mental health. The Report recommends that the Government optimise the digital space to encourage help-seeking behaviour and enhance the uptake of digital therapies and telehealth services.
It called on the Government to provide more incentives to public organisations and private enterprises to improve employees’ mental health literacy and encourage help-seeking behaviour. Employers should be encouraged to provide workplace mental health assessment and provide training for managers to accommodate employees in need, and provide early intervention services.
In line with the World Health Organization’s framework on enhancing mental health system policy, the Report calls on the Government to empower a governmental unit with evaluation, design, and executive capability. The unit should set measurable key performance indicators, regularly collect data, evaluate the effectiveness of existing programmes, and develop updated policy plans and programmes. The unit should also put forward clear timetables and resource allocation plans to translate policy into actionable plans and programmes.
Speaking at the launch of the Report, OHKF Executive Vice Chairman Mr Bernard Charnwut Chan said: “The corporate sector is a key partner in the city’s mental health support and response system. A resilient and productive workforce is a critical part to the city’s vibrancy and competitiveness, especially when Hong Kong starts reopening to the rest of the world.” This is why a public forum was held today to pool the wisdom of relevant sectors including the corporate sector who have both the incentives and the good will to promote workplace mental health.
The University of Hong Kong’s Chi-Li Pao Foundation Professor in Psychiatry Professor Eric Chen Yu-hai said: “Psychiatrists and clinical psychologists are key service providers in Hong Kong’s mental health system, but the city has long suffered from the under-supply of these professionals. This Report not only provides concrete recommendations to overcome this manpower shortage, but also looks beyond specialist care to optimise the provision of mental health services. It is important to fully leverage the private sector general practitioners and family medicine specialists, as well as mobilising resources outside of the hospital setting such as District Health Centres and social services and NGO programmes to provide frontline mental healthcare. These proposals are timely and should be at the forefront of every policymaker’s mind to help improve our city’s overall wellbeing.”
The University of Hong Kong’s Henry G. Leong Professor in Social Work and Social Administration Professor Terry Lum said: “The challenges that social workers and social services face in the field of mental health are numerous, particularly as patient volumes increase. The Report calls on the Government to upskill social workers with training that would leverage them in clinical psychological service settings. Furthermore, with Integrated Community Centres for Mental Wellness having run for over a decade, the Report urges the Government to conduct a service review of the centres to provide integrated care that matches the emerging population needs. These recommendations are indispensable in creating a sustainable mental health ecosystem for Hong Kong.”
Full Report of Towards a Fit-for-Purpose Mental Health System:
Full report:http://bit.ly/3Y8kmt0
English Executive Summary:https://bit.ly/3ux2zhF
Chinese Executive Summary:https://bit.ly/3Y39ZH4









